What is eczema?
Eczema (atopic dermatitis) is a recurring, inflammatory, non-infectious skin condition that affects one in three Australians at some stage throughout their lives. This skin condition is most common in people with a family history of an atopic disorder, which includes hay fever or asthma.
Usually appearing in early childhood, patches of skin become red, scaly and itchy. In severe eczema cases, there may be weeping, bleeding or crusting over of the skin patches. This skin condition can flare and subside for no apparent reason, causing the eczema sufferer a lot of discomfort and pain.
Weeping skin can occur when the atopic dermatitis has become infected, usually with the bacterium Staphylococcus aureus (‘golden staph’). It’s important to note that eczema is not contagious.
While eczema affects all ages, it generally materialises in early childhood (in babies between 2 to 6 months of age) and can improve with age. A small percentage of eczema sufferers can experience severe eczema into adulthood. Adult eczema can be very hard to treat as it’s often caused by factors including medications. While eczema can be effectively managed and treated, there are no cures currently available.
Are you considering participating in a clinical trial?
Patient participants with a disease or condition may decide to participate in clinical trials to contribute to better understanding of, or better treatment or a potential cure for their disease or condition. In some cases, clinical trials can provide access to new interventions before they are widely available.
Trials also offer the hope of developing better interventions or tests for a particular disease or condition, so that even if a trial does not provide a benefit for an individual, it may provide benefits for others with the disease in the future.
As a patient participant, even when you receive the highest quality care, you may also benefit from additional support and attention provided by clinical trial staff who understand your disease or condition (source: australianclinicaltrials.gov.au)
We are currently enrolling adult and adolescent participants for a clinical study focused on eczema. This study aims to assess the effectiveness and safety of a novel oral medication in adolescents with eczema. If you're interested in learning more about this study or registering, please click here.
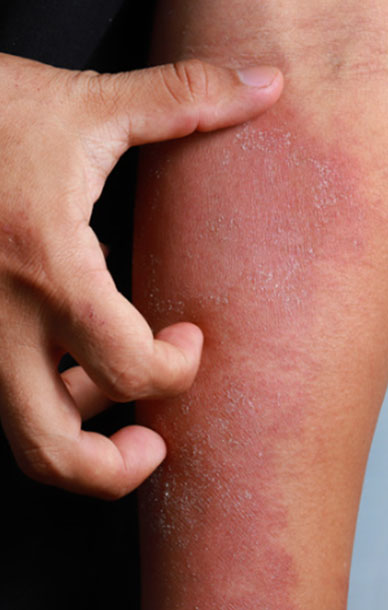
Causes of eczema
Even though people with eczema can have or will develop other allergies, (suggesting that inherited factors increase the tendency to develop eczema) it doesn’t mean that allergies will result in someone developing eczema.
Eczema results from an inability to repair damage to the skin barrier that has been caused by a gene mutation which leads to inability to form an important skin protein called filaggrin. If people have a mutation in the gene for producing filaggrin, the skin barrier will not be formed completely. Usually every cell in the skin will have two copies of the gene producing filaggrin. For people who are susceptible to eczema they only have one copy of this gene.
While you only need only one copy of the gene to create a normal skin barrier, two copies are vital for skin barrier repair. A person with only one copy of the filaggrin coding gene may find that their ability to repair the skin barrier is limited when their skin is exposed to irritants or their skin barrier is disrupted.
The skin barrier in people who have eczema is different from those people who do not have eczema. In people with eczema the skin barrier does not work as well. The skin has less water retaining properties, so the moisture is easily lost from the skin, causing it to dry out easily. Increasing the amount of water intake will not rectify this. While the exact cause of eczema is unknown it appears to be linked to the following internal and external triggers:
Internal
- A family history of eczema, asthma or hay fever is the strongest predictor of a child developing eczema. If both parents have eczema, there will be an 80% chance that their children may develop eczema
- Some foods and alcohol including dairy and wheat products, citrus fruits, eggs, nuts, seafood, chemical food additives, preservatives and colourings
- Stress
External
- Environmental irritants including tobacco smoke, chemicals, weather (hot and humid or cold and dry conditions), air conditioning or overheating
- Allergens including house dust mites, moulds, grasses, plant pollens, foods, pets and clothing, soaps, shampoos and washing detergents
Types of eczema
Infantile Eczema
Usually starts in the first 6 months of life. Symptoms include an itchy, red and dry rash on the skin. Infantile eczema usually improves significantly between the ages of 2 to 5 years.
Childhood Eczema
Can start after infantile eczema or appear for the first time between the ages of 2 to 4 years. The dryness and rash are usually found behind the knees, in the creases of the elbows and across the ankles. It may also involve the neck, ears and face. This type of eczema usually improves with age. While most children will completely outgrow their eczema, some continue with a tendency for sensitive and dry skin into adulthood.
Adult Eczema
Is similar to that of older children where areas of very dry, itchy, reddened skin form at the elbow creases, wrists, neck, ankles and behind the knees. This skin may also weep. Adult eczema can improve in middle age and usually resolves in older age.
Symptoms of eczema
Eczema affects the skin, causing itching, redness and oozing of the skin. Patients report that eczema is usually itchy. For many people, this itch is only mild. However, sometimes it can increase in intensity resulting in extremely inflamed skin.
Some eczema patients find that the itch gets so bad that they scratch it until it bleeds. This is called the “itch-scratch cycle” and can make your eczema worse. Over time your skin may also get rough and thickened.
As a skin disease, eczema can improve or get worse over days, weeks or months. If eczema gets worse, it’s called an eczema flare – this can happen without a single factor being responsible for it.
Eczema and its symptoms are different for everyone. Your eczema may not look the same on you as it does on your child or another adult. Eczema can also appear in different areas of your body at different times.
Symptoms of eczema can include:
- Dry, sensitive skin
- Red, inflamed skin
- Moderately to severely itching skin
- Rashes that are red, dry, patchy or cracked. While they can appear on any body part they commonly appear on the face, neck, inner elbows, hands, backs of ankles or knees.
- Dark coloured patches of skin
- Rough, leathery or scaly patches of skin
- Oozing, crusting or swelling skin
- Skin that is weeping watery fluid
- Rough, “leathery” or thick skin
You may only have a few of these eczema symptoms or all of them. It’s important to note that the only way to know if you have eczema is to visit your doctor or dermatologist so they can look at your skin and ask about your symptoms.
Triggers of eczema
If you have eczema it means that when your skin barrier is damaged, the moisture evaporates resulting in your skin being more susceptible to allergens and irritants. This irritation can trigger your skin to release certain chemicals that make the skin itchy. If you scratch the skin, more chemicals are released which results in the skin feeling even itchier. This is known as the “scratch and itch” cycle and can be very distressing.
Known triggers and aggravating factors for eczema include:
- Dry skin
- Scratching (wearing gloves at night or clipping fingernails short may be with young children)
- Viral or bacterial infections
- Swimming in chlorinated swimming pools
- Playing in sand and particularly sandpits or sitting directly on carpets or grass
- Inhalant allergens. Eczema can become worse in spring and summer because of pollen sensitivity
- Food intolerances to artificial colour and preservatives
- Irritants such as perfumes, soap, chemicals, woollen or synthetic fabrics
- Temperature changes (such as heat) or overly heated rooms
- Stress (this can make it worse but it’s important to note that eczema is not a psychological condition).
These eczema triggers may be relevant for some people, but it’s not routinely recommended that everyone avoid all these potential triggers. You should discuss these potential triggers with your doctor or dermatologist.
Coping with eczema - general
If you have skin that’s affected by eczema it can be more vulnerable to infections including warts, cold sores and impetigo. Good hygiene suggestions include:
- Only having lukewarm baths and showers as hot baths and showers can aggravate your eczema.
- Use soap free products like sorbolene cream to wash your body and face.
- Avoid wearing scratchy materials close to your skin including pure wool, acrylic or polyester. A cotton and synthetic mix can be the best material for eczema patients. It’s also useful to remove labels from your clothing to avoid itching.
- After a shower or bath, pat your skin dry rather than rubbing it dry with a towel.
- Avoid overheating your skin at night. Use several layers of blankets instead of one heavy layer.
- Keep your fingernails as short as possible. Having longer nails means you’ll be more likely to injure your skin if you scratch.
- Consider installing a water-softening device if the water in your area is ‘hard’ (full of minerals) or alkaline.
- Because seawater is known to reduce the symptoms of eczema, swimming in the sea can be helpful.
- Use a moisturiser every day to prevent your skin from cracking, itching or to offer relief. Having well moisturized skin will also help block out germs that cause infections.
- Even hypoallergenic cosmetics can irritate your skin. Whenever possible, it’s good to keep your face free of make-up.
- Avoid wearing fragranced skin lotions, perfumes and strongly scented shampoos.
- When you want to use a new cosmetic, we suggest you try it on a small, inconspicuous area of skin such as your forearm. If you experience a reaction, it’s best not to use the product again.
Coping with eczema - if you have allergies
Some eczema patients can have an allergic reaction to environmental triggers. It can be helpful for some people to have allergy testing (for example, prick testing for common environmental allergens such as house-dust mites, moulds and grass pollens). If you suspect you may have this allergy, ask your doctor or dermatologist for more information.
The best way to cope with temperature changes if you have eczema
If you have eczema, abrupt temperature changes and humidity changes can sometimes irritate your skin. For example, going in and out of air-conditioned buildings on hot days or heated buildings on cold days. Some patients report that physical activity or exercise that makes you sweat heavily can also trigger the itch of eczema.
We suggest that you:
- Don’t overheat your house in winter. Dress warmly when going outside but remove the extra layers when inside.
- Avoid making your house too cool in summer. Air conditioners can dry out the air and irritate your skin.
- Avoid hard physical activity in hot weather.
Treatment for eczema
It is very important to seek professional medical advice before using any medication: whether over the counter or prescription to determine its side effects.
Eczema treatments include:
- Topical corticosteroids are the most common form of eczema treatment that helps reduce inflammation and itchiness. Most topical corticosteroids are available on prescription; however, some milder strength ones are available in the pharmacy. In severe cases of eczema, a short course of oral corticosteroids may be necessary. This must be done under careful medical supervision because symptoms may become worse once you have finished taking the tablets.
- Sedating antihistamines can induce sleep and reduce itchiness.
- Applying bandages can soothe the skin to reduce itchiness and help heal lesions.
- Antibiotics can treat secondary infections.
- Ultraviolet radiation therapy (phototherapy)
- Emollients (moisturisers) – you may need to try different brands until you find an emollient that is right for you. Your dermatologist or doctor will be able to advise you on the best emollients to use.
What anti-inflammatory ointments treat eczema?
Eczema responds well to anti-inflammatory creams. Topical steroids (corticosteroids) come in various strengths and are available by prescription from your doctor. It is recommended that you use the lowest strength topical steroid cream that works adequately. Using high-strength topical steroids for extended periods, especially on delicate areas like the face, can cause side effects, which include thinning of the skin. After bathing, make sure your skin is thoroughly dry before applying the cream.
In addition, non-steroid anti-inflammatory creams can help reduce flare-ups of eczema if applied at the first signs of eczema.
Coal tar can be applied to the affected areas to reduce the itch from eczema. Only use it under supervision of a doctor who is experienced in managing eczema. Coal tar has a strong smell and usually stains any fabric it touches. It can also irritate some people’s skin.
Using ultraviolet radiation therapy to treat eczema
Ultraviolet radiation therapy (phototherapy) for eczema can help reduce the symptoms of chronic eczema. Exposure under medical supervision can be carefully monitored with the use of specially designed ‘cabinets’. The patient stands naked in the cabinet as the fluorescent tubes emit ultraviolet radiation.
People with stubborn eczema may need up to 30 sessions. The risks of unsupervised ultraviolet radiation therapy can be the same as for sunbathing – faster ageing of the skin and greater risk of skin cancer.
Using oral anti-inflammatory medication to treat eczema
Most people affected by eczema can manage the condition using ointments and creams. While oral medications can help people, whose eczema is resistant to treatment, their side effects can include high blood pressure, increased susceptibility to all types of infections, and mood and behavioural changes.
Because of these risks, and the need for close and regular monitoring, oral anti-inflammatory treatment is only considered in severe cases of eczema that are difficult to control with other therapies.
The importance of eczema treatment
There is growing evidence that allergens introduced into the body through the skin can lead to the later development of food allergy, asthma and hay fever. Aggressively treating eczema in children and taking steps to restore normal skin barrier function might lower the future risk of these conditions.
What are the complications of having eczema?
As skin with eczema lesions is often broken, it places the sufferer at risk of contracting skin infections. At the first sign of any infection, professional medical advice should be sought.
Eczema sufferers are also at risk of developing herpes simplex type 1 (cold sores) which can spread over a large area of the skin. Because herpes simplex can spread over wide areas, it’s important to see your doctor for prompt treatment.
Warts (small, raised lumps) can be caused by viral infections. They can take up to 12 months to clear themselves up.
People with eczema are also at risk of contracting a widespread skin infection known as impetigo (school sores). Treatments for this include antibiotic tablets and antiseptic creams.
To avoid any complications associated with vaccination, the disease should be discussed with a medical professional. Normal childhood immunizations generally pose no risk to the eczema sufferer.
To book a consultation please call us on 9654 2426 or email appointments@sinclairdermatology.com.au
Why Choose Sinclair Dermatology?
Leader in skin and hair loss treatment and research
More than 50% of dermatology research papers in Australia are published by our team
Largest dermatology clinical trial research centre in Australia
Only medical centre in Australia to use 3D whole body imaging technology to map moles and lesions for skin cancer detection.
 Onsite pathology and compounding pharmacy
Onsite pathology and compounding pharmacy Our dermal clinic uses state of the art laser machines
Our dermal clinic uses state of the art laser machines




