Psoriasis is an inflammatory skin condition that can result in extreme discomfort and irritation. It is not contagious with symptoms including red scaly patches on skin, itchiness and flaking of the skin.
What is psoriasis?
Psoriasis is a noncontagious, inflammatory chronic skin condition that is characterized by skin inflammation and flaking. This skin condition occurs because skin cells grow or turnover too quickly.
Inflammatory chemicals produced by specialized white blood cells called lymphocytes trigger the proliferation of skin cells. Psoriasis commonly affects the skin of the elbows, knees, and scalp but can occur anywhere on the body.
Psoriasis is an incurable, chronic inflammatory skin condition that can be treated. It has a variable course, periodically worsening and improving. Psoriasis can unexpectedly clear for years and stay in remission.
Are you considering participating in a clinical trial?
Patient participants with a disease or condition may decide to participate in clinical trials to contribute to better understanding of, or better treatment or a potential cure for their disease or condition. In some cases, clinical trials can provide access to new interventions before they are widely available.
Trials also offer the hope of developing better interventions or tests for a particular disease or condition, so that even if a trial does not provide a benefit for an individual, it may provide benefits for others with the disease in the future.
As a patient participant, even when you receive the highest quality care, you may also benefit from additional support and attention provided by clinical trial staff who understand your disease or condition (source: australianclinicaltrials.gov.au)
We're in the process of recruiting patients for a clinical study targeting psoriasis in adults. This study is designed to evaluate the efficacy and safety of an innovative oral treatment for adolescents with psoriasis. If you're interested in finding out more or participating in this study, please click here.
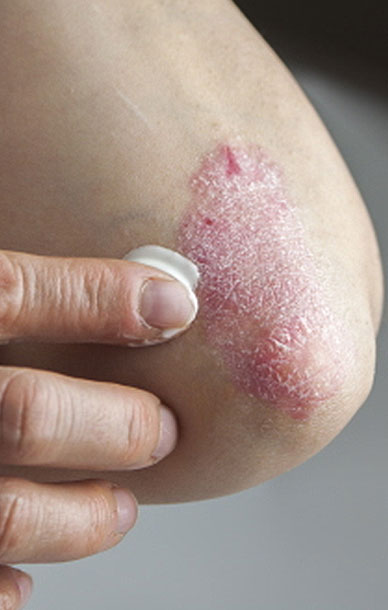
Causes of psoriasis?
Research has shown that while 10% of the population can inherit at least one of the genes for psoriasis, only 2-3% of the population is troubled with the scaling skin disorder. This indicates that you need to have the right combination of genes to develop psoriasis. If both your parents have a number of psoriasis genes, you may develop psoriasis.
Psoriasis is thought to be an immune system disorder, where your white blood cells collect in the skin and release inflammatory mediators (chemicals which produce inflammation). This causes your skin to get red and thicker than usual.
Some genetic markers have been linked to psoriasis and may be important in the development of the disease, however, not all people with these markers develop psoriasis. One theory is that people who have inherited a genetic susceptibility to psoriasis have the condition triggered by an external factor. Some of the proposed external factors include stress, infection, smoking, medications, injury, alcohol and obesity.
Factors that cause your genes to become activated include:
- Infections (particularly strep but possibly Candida in some people)
- Stress or irritation
- Smoking
- Medications including lithium, beta blockers, non-steroidal anti-inflammatory medications and antimalarial drugs
- Injury
- Chemical reaction, particularly on the elbows, hands and knees
- Obesity
People with HIV/AIDS (especially in the later stages of the disease) can also develop psoriasis. It tends to be more severe in HIV patients with these sufferers reporting a family history of the condition.
Types of psoriasis
The spectrum of psoriasis ranges from mild with a limited involvement of small areas of skin to large, thick plaques to red inflamed skin affecting the entire body surface.
Types of psoriasis include:
- Plaque psoriasis – the most common form of psoriasis
- Pustular psoriasis – a more severe form of psoriasis that can be painful
- Guttate psoriasis – found mostly in children
- Napkin psoriasis – characteristically seen in infants between 2 and 8 months of age
- Flexural psoriasis – affecting body folds and genital areas
- Erythrodermic psoriasis – a severe form requiring hospitalisation.
Symptoms of psoriasis
People affected by psoriasis may have the following effects that include:
- Thick red or silvery scaly patches of skin on their scalp, elbows, knees and other parts of the body,
- Itchy skin, however some people with psoriasis do not feel itchy
- Dry or cracked skin,
- Thickened and ridged fingernails and toenails,
- Stiff or sore joints (an indication of psoriatic arthritis)
Effects of psoriasis
If you have psoriasis it can be uncomfortable, embarrassing and affect your self-esteem. To reduce the visibility of flakes on your clothes, it is helpful to wear lighter coloured clothing, instead of dark colours. Women can be more affected by psoriasis psychologically than men.
Psoriasis can also affect your physical health. A number of people with psoriasis also develop a type of arthritis, called psoriatic arthritis.
What is psoriatic arthritis?
For an unknown reason, psoriasis can cause a form of arthritis known as psoriatic arthritis. The symptoms include:
- Discomfort, throbbing or swelling in one or many joints
- Tenderness in any joint
- Pain caused by inflammation in the joints, which stimulates nerve endings
- The joints most likely to be affected are the last joint in the fingers or toes, the sacrum (lower back), wrists, knees or ankles.
While there is no cure for psoriatic arthritis, it can be managed with medications and by keeping active and exercising regularly. As with many types of arthritis, there could be flare-ups.
Psoriasis patients also have a higher risk of heart attacks and strokes. If you have psoriatic arthritis you may be referred to a rheumatologist, who specialises in arthritis, to decide the best course of treatment.
Treatment for psoriasis
While several treatment options exist for psoriasis, there is no cure for this skin condition. The type and strength of treatment depends on the severity of the disease. Doctors may prescribe a range of treatments for the relief of psoriasis symptoms including:
- Topical psoriasis treatments including coal tar preparations, cortisone and other prescription creams
- Ultraviolet light therapy
- Systemic drug therapy medications
- Lifestyle changes
Topical psoriasis treatments:
These treatments are usually the most popular treatment option for psoriasis with topical steroids and tar products being the most popular treatments. This psoriasis treatment involves applying creams and ointments to the affected area of skin. Some of these topical psoriasis treatments are available over the counter without a prescription.
The most effective creams contain a corticosteroid, which treats the immune system and the inflammatory response occurring in the region where the psoriasis lesions are. It is very important to seek the advice of your doctor or dermatologist before you use a topical psoriasis treatment.
Other types of creams and ointments that are available include vitamin D (calcipotriol) creams, coal tar-based shampoos and creams and vitamin A treatments (retinoids). These have varying effectiveness with the treatment of psoriasis.
Light therapy (phototherapy) psoriasis treatment:
In moderate cases of psoriasis, UV light can be used to effectively treat psoriasis. Different types of UV light your dermatologist may use include PUVA (psoralen plus Ultraviolet A light) and Narrow Band UVB.
Systemic drug therapy:
This type of psoriasis treatment is usually used for people with severe cases of psoriasis. There are various well known oral medications used for the treatment of psoriasis.
Biologic therapies have revolutionised the treatment of psoriasis and target the specific parts of the immune system involved in causing psoriasis. Because these treatments are expensive, the government only subsidises the cost for patients with severe cases of the disease and where all other treatment options have been exhausted.
If you take any of these medications, it is very important to have regular check-ups with your dermatologist or doctor to monitor for side effects.
Lifestyle changes to treat psoriasis:
Smoking can make your psoriasis worse, so quitting (or the very least, cutting down) can help to control your psoriasis symptoms. It is also helpful to exercise regularly and eat a healthy and well-balanced diet.
Moisturisers may help improve your psoriasis and make it more comfortable. Because stress is a key factor for some people with psoriasis, learning to manage and reduce stress where possible can also be helpful.
To book a consultation please call us on 9654 2426 or email appointments@sinclairdermatology.com.au
Are you considering participating in a clinical trial?
Patient participants with a disease or condition may decide to participate in clinical trials to contribute to better understanding of, or better treatment or a potential cure for their disease or condition. In some cases, clinical trials can provide access to new interventions before they are widely available.
Trials also offer the hope of developing better interventions or tests for a particular disease or condition, so that even if a trial does not provide a benefit for an individual, it may provide benefits for others with the disease in the future.
As a patient participant, even when you receive the highest quality care, you may also benefit from additional support and attention provided by clinical trial staff who understand your disease or condition (source: australianclinicaltrials.gov.au)
If you would like to hear more or take part in a Psoriasis trial, please click here: expression of interest form
Why Choose Sinclair Dermatology?
 Leader in skin and hair loss treatment and research
Leader in skin and hair loss treatment and research More than 50% of dermatology research papers in Australia are published by our team
More than 50% of dermatology research papers in Australia are published by our team Largest dermatology clinical trial research centre in Australia
Largest dermatology clinical trial research centre in Australia Only medical centre in Australia to use 3D whole body imaging technology to map moles and lesions for skin cancer detection.
Only medical centre in Australia to use 3D whole body imaging technology to map moles and lesions for skin cancer detection. Onsite pathology and compounding pharmacy
Onsite pathology and compounding pharmacy Our dermal clinic uses state of the art laser machines
Our dermal clinic uses state of the art laser machines




